The first stage of the state’s planned conversion of the Workers’ Compensation Official Medical Fee Schedule (OMFS) to a reimbursement system similar to the one used in Medicare would boost annual payments to physicians who treat injured workers between $56 million and $157 million according to an analysis by the California Workers’ Compensation Institute. SB 228, passed by state lawmakers in 2003, required the Division of Workers’ Compensation (DWC) to update the physician portion of the OMFS, starting in 2004 with a 5% reduction in any of the maximum physician fees that exceeded Medicare rates, provided that such reductions did not take the fees below Medicare levels. Thereafter, SB 228 required the state to adjust the fees as Medicare rates changed, and as of January 1, 2006, it gave the DWC authority to adopt a new schedule for physician services. DWC has now begun that process, focusing initial efforts on converting some of the most commonly used office visit codes in the physician portion of the OMFS to a Resource-Based Relative Value Scale (RBRVS) schedule. In contrast to the current schedule, which bases allowable fees for physician services on historical charges, an RBRVS schedule would parallel the Medicare payment structure, basing maximum reasonable fees on a physician’s work (time and skill required), practice expense (staff time and overhead costs), and malpractice expense. Unlike the current OMFS, which uses Current Procedural Technology (CPT) codes that are more than 10 years out of date, an RBRVS schedule would allow medical providers to bill with current CPT codes the way they do in all other venues, and would simplify and streamline medical bill review and adjudication. While the DWC intends to study a complete OMFS conversion to Medicare RBRVS rates later this year, the proposed first step is limited to increasing allowable fees for 10 common E&M office visit codes that pay less than Medicare. The overall effect on workers’ compensation medical payments was unknown, however, because differences between the current OMFS maximums and the Medicare rates for these 10 office visit codes not only vary by code, but by geographic regions within the state, as Medicare bases its fees on local costs, and has 9 regional fee schedules in California. At the Division’s request, CWCI reviewed claims data from its Industry Claims Information System (ICIS) to estimate the impact of these changes on payments. The claim sample encompassed about 1 million E&M office visit codes with 2005 dates of service. Although there are 73 distinct E&M codes in the OMFS, the analysis found that the 10 E&M office visit codes targeted for the increase comprise 80 percent of all E&M services used in California workers’ comp, and two-thirds of the total amount paid for E&M services. Of the estimated $2.4 billion in total California workers’ comp payments to physicians in 2005, the Institute estimated payments for all E&M services totaled $508 million, of which the 10 office visit E&M services accounted for $342 million. After using ICIS to estimate how much was paid for the 10 E&M office visit categories under the current schedule, the Institute calculated how much would have been paid for those 10 codes using California’s nine regional Medicare fee schedules, and a tenth option: a weighted, regionally adjusted average reimbursement plan, based on the geographic mix of E&M services from the sample.
Comparing the estimated $342 million paid under the 2005 OMFS for the 10 E&M office visit codes to what would have been paid under the 10 alternative schedules showed that the Medicare E&M office visit fees for all regions were significantly above the corresponding rates allowed under the current OMFS.
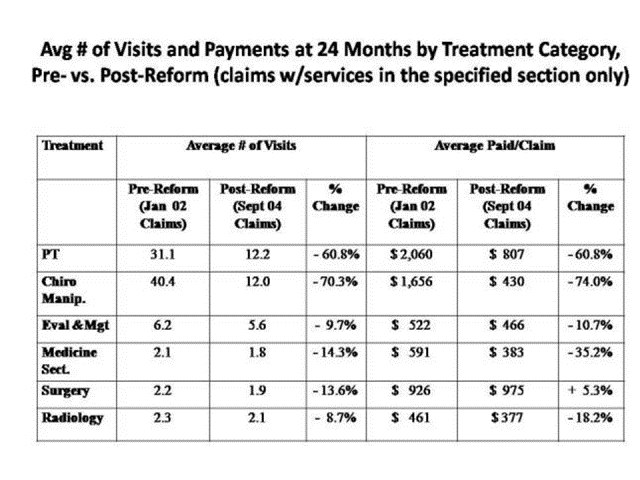
The estimated system-wide increases ranged from $56 million more per year (+16.4 percent) if the “Rest of California” fee schedule were applied uniformly across the state to $157 million more (+46.1 percent) if the Santa Clara region fee schedule were applied statewide. The regionally adjusted Medicare weighted average would add an estimated $79 million in E&M payments. The analysis on the impact of applying Medicare rates to the 10 workers’ comp E&M office visits is in the Research section of CWCI’s website at www.cwci.org. CWCI’s written comments on the proposed rules and regulations also are posted as testimony in the Regulatory section of the website. The comments feature a broader analysis that looks at the potential reimbursement effects for all 73 E&M codes under the 9 regional fee schedules Medicare now uses in California, as well as the regionally adjusted Medicare weighted averages.