The average amount paid to a California workers’ compensation treating physician for a medical report fell more than 30 percent in the first quarter of 2014 as the state began to transition to a Resource-Based Relative Value Scale (RBRVS) fee schedule, though a CWCI analysis traces the decline to changes in how various evaluation and management (E/M) services are reimbursed rather than reductions in the fees assigned to the report codes.
California’s transition to an RBRVS fee schedule that began a year ago led to 2 changes affecting physician reporting: 1) consulting physician evaluation services are now billed using an initial visit code, and associated reports are no longer separately reimbursable unless requested by the DWC Administrative Director, the Appeals Board or a Qualified Medical Evaluator in the context of a med-legal evaluation; and 2) the reimbursement to the primary treating physician for medical records review outside the context of a face-to-face E/M service has been bundled into the face-to-face E/M service fee, and there is no longer a separate allowance for a prolonged service fee.
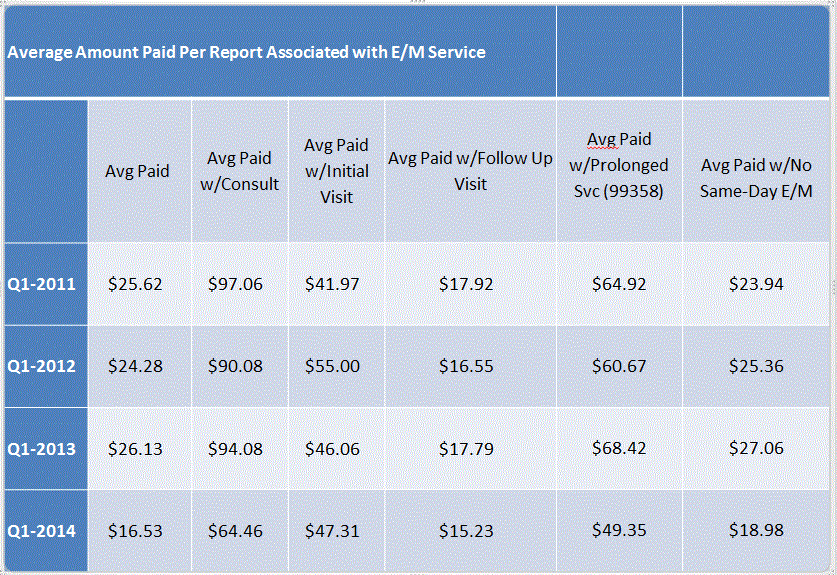
To monitor how physician reporting changed after these changes took effect, CWCI Senior Research Associate Stacy Jones compared data on medical reports for service dates from the first quarter of 2014, when the transition to the new schedule began, to corresponding data from the first quarters of 2011, 2012 and 2013, when the old fee schedule was still in effect. After determining the average amounts paid and the distribution of reports by the nature of the underlying E/M service (i.e., reports associated with initial visits, consultations, follow-up visits, prolonged services), Ms. Jones found that while the average amount paid for all physician reports fell more than 30 percent under the RBRVS fee schedule, the changes in the average reimbursements varied dramatically by type of report.
Comparing the mix of reports associated with the various E/M services revealed that after the rules changed under the new schedule, relatively inexpensive reports on follow-up visits increased from 78 percent to 86 percent of all physician reports, while the biggest declines were in consultation and prolonged service reports, which historically received the highest reimbursements. Consultation reports, which had represented 6 percent of physician reports under the old schedule, and prolonged service reports, which had accounted for 4 percent, both dwindled to less than 1 percent of all reports after the RBRVS schedule took effect. Thus, the initial results on physician reporting following adoption of the new schedule indicate that the change in the mix of reports has been the key factor in reducing the average amount paid for physician reports.
CWCI will continue to monitor the volume, distribution and reimbursement of physician reports in California workers’ comp as more developed data become available. In the meantime, the Institute has published a Research Update report, “Changes in Workers’ Compensation Physician Reporting Under California’s RBRVS Fee Schedule: Initial Results,” which provides additional details and graphics from the latest study. The Research Update report is available to CWCI members and subscribers in the Research section at www.cwci.org.